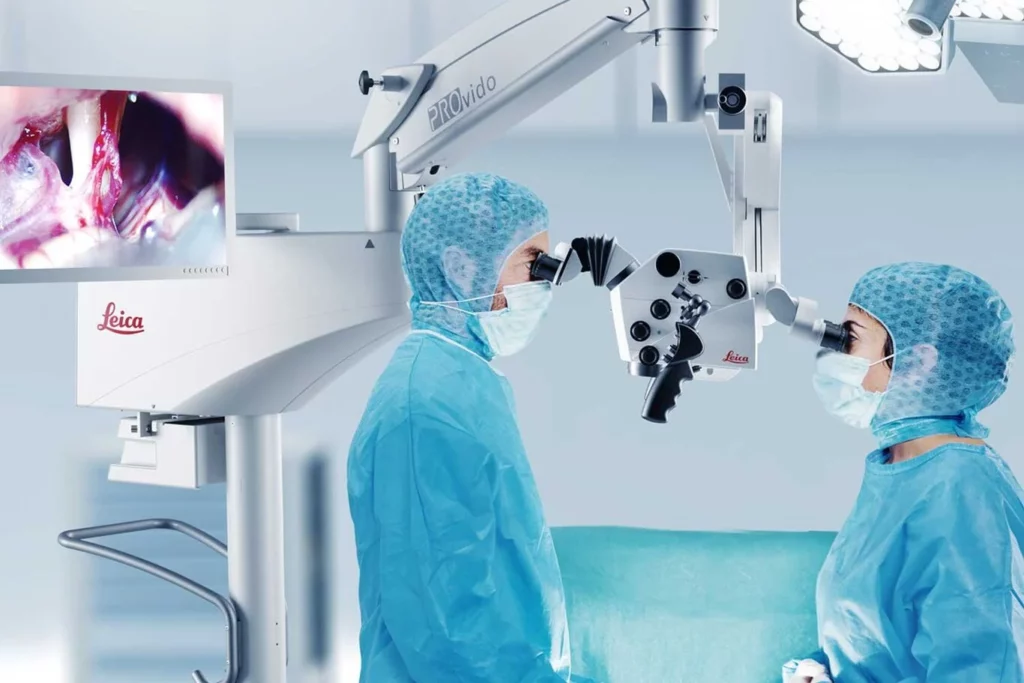
When investing in surgical equipment, precision, reliability, and cost-effectiveness are key considerations. For many healthcare facilities, acquiring a pre-owned Leica surgical microscope presents a strategic advantage, offering world-class optics and advanced technology at a fraction of the cost of new units. At DB Surgical, we specialize in providing high-quality pre-owned Leica surgical microscopes, ensuring that medical professionals can access the best equipment without compromising their budget or performance standards.
When investing in surgical equipment, precision, reliability, and cost-effectiveness are key considerations. For many healthcare facilities, acquiring a pre-owned Leica surgical microscope presents a strategic advantage, offering world-class optics and advanced technology at a fraction of the cost of new units. At DB Surgical, we specialize in providing high-quality pre-owned Leica surgical microscopes, ensuring that medical professionals can access the best equipment without compromising their budget or performance standards.
Here’s why a pre-owned Leica surgical microscope might be the perfect solution for your practice or facility.
1. Significant Cost Savings Without Compromising Quality
Surgical microscopes represent a substantial investment, with new units often costing hundreds of thousands of dollars. Opting for a pre-owned Leica microscope allows facilities to save up to 50% or more compared to new models while still benefiting from Leica’s industry-leading optical performance and ergonomic design.
At DB Surgical, we meticulously inspect, refurbish, and certify every pre-owned Leica microscope to ensure it meets or exceeds OEM specifications. This means you receive a top-tier surgical microscope with proven reliability at a much lower cost.
2. Immediate Availability for Faster Implementation
New surgical microscopes can have long lead times due to production and supply chain delays. This can be a major challenge when upgrading or expanding surgical capabilities.
With pre-owned Leica microscopes from DB Surgical, you gain immediate access to the technology you need, minimizing downtime and enabling your team to enhance surgical precision without unnecessary delays. Our inventory is ready to ship, ensuring your OR remains fully operational.
3. High-Quality Optics & Advanced Features
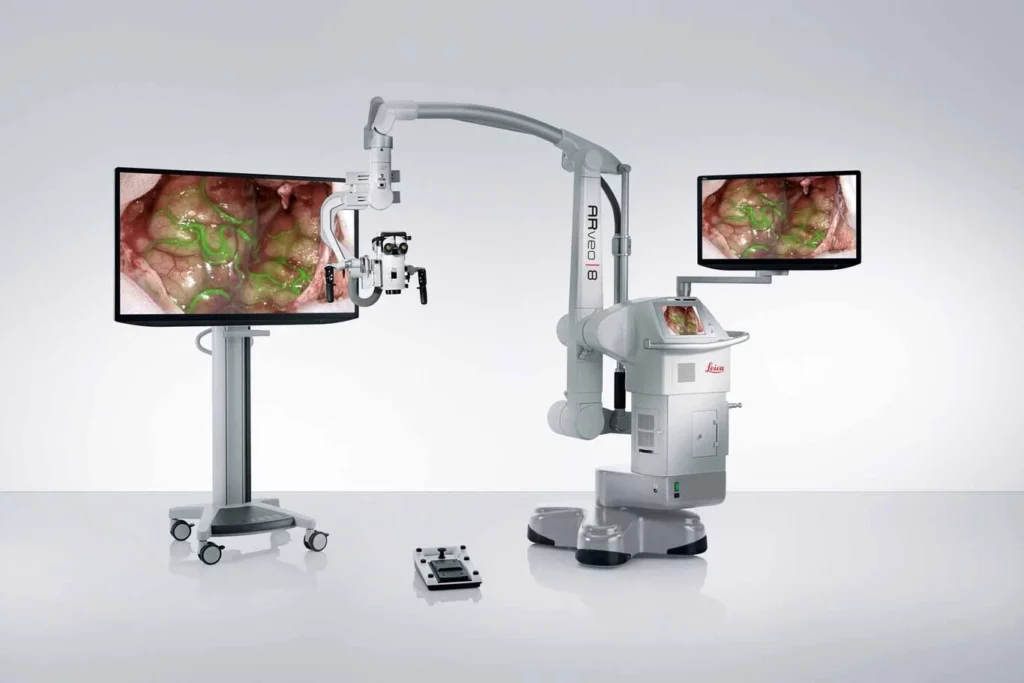
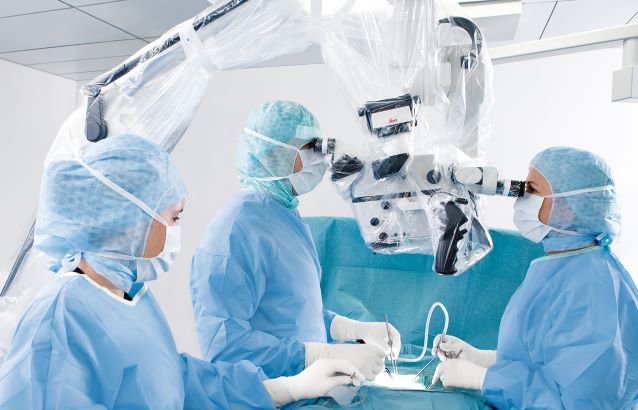
Leica microscopes are known for their exceptional optical clarity, fluorescence imaging capabilities, and ergonomic designs, enabling surgeons to perform intricate procedures with greater precision and ease. When purchasing a pre-owned Leica surgical microscope from DB Surgical, you still gain access to:
- Apochromatic optics for superior resolution and depth of field
- FusionOptics technology for enhanced visualization
- Integrated recording and digital imaging options for documentation and education
- Ergonomic designs to reduce surgeon fatigue
Our expert team ensures that all pre-owned Leica microscopes are fully functional and calibrated, so you experience the same high performance you’re accustomed to.
4. Environmentally Responsible & Sustainable Choice
Purchasing pre-owned medical equipment isn’t just financially smart, it’s also an environmentally responsible choice. By extending the lifespan of high-quality surgical microscopes, healthcare facilities can reduce electronic waste and lower their carbon footprint.
DB Surgical is committed to sustainable solutions by refurbishing, repurposing, and reintroducing high-performance surgical technology into the market, helping facilities meet both financial and environmental goals.
5. Flexible Financing & Service Support
At DB Surgical, we understand that capital budgets can be tight, and financial flexibility is crucial. That’s why we offer:
- Competitive financing options to spread out cost
- Extended warranties and service plans for peace of mind
- Expert technical support and bespoke disposable drapes to ensure your microscope continues to perform at its best
Our team is dedicated to providing white-glove services from selecting the right microscope to installation and ongoing support.
Unlock Value with a Pre-Owned Leica Surgical Microscope from DB Surgical
When it comes to surgical excellence, Leica microscopes set the standard and with a pre-owned unit from DB Surgical, you can achieve the same superior performance at a fraction of the cost.
If you’re considering upgrading your surgical microscope or expanding your OR capabilities, contact us today to explore our inventory of pre-owned Leica surgical microscopes. We offer same-day shipping, competitive financing, and expert service to ensure you receive the best value without compromise.
Call us or visit our website to learn more.


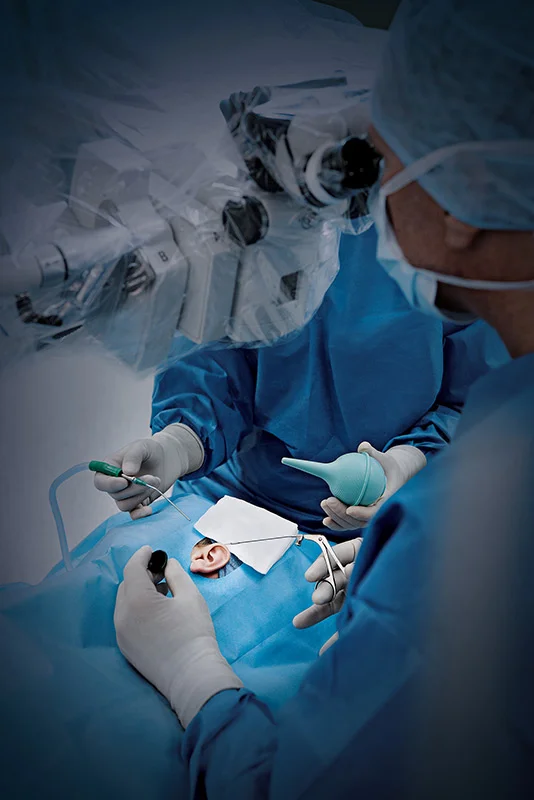 The Importance of Precision in ENT Surgery
The Importance of Precision in ENT Surgery